Bacterial Oncotraits Rather than Spatial Organization Are Associated with Dysplasia in Ulcerative Colitis (Journal of Crohn's and Colitis)
Bacterial Oncotraits Rather than Spatial Organization Are Associated with Dysplasia in Ulcerative Colitis
Carlijn E Bruggeling, Maarten te Groen, Daniel R Garza, Famke van Heeckeren tot Overlaer, Joyce P M Krekels, Basma-Chick Sulaiman, Davy Karel, Athreyu Rulof, Anne R Schaaphok, Daniel L A H Hornikx, Iris D Nagtegaal, Bas E Dutilh, Frank Hoentjen, Annemarie Boleij
Background and Aims
Colonic bacterial biofilms are frequently present in ulcerative colitis [UC] and may increase dysplasia risk through pathogens expressing oncotraits. This prospective cohort study aimed to determine [1] the association of oncotraits and longitudinal biofilm presence with dysplasia risk in UC, and [2] the relation of bacterial composition with biofilms and dysplasia risk.
Methods
Faeces and left- and right-sided colonic biopsies were collected from 80 UC patients and 35 controls. Oncotraits [FadA of Fusobacterium, BFT of Bacteroides fragilis, colibactin [ClbB] and Intimin [Eae] of Escherichia coli] were assessed in faecal DNA with multiplex quantitative polymerase chain reaction [qPCR]. Biopsies were screened for biofilms [n = 873] with 16S rRNA fluorescent in situ hybridiation. Shotgun metagenomic sequencing [n = 265], and ki67-immunohistochemistry were performed. Associations were determined with a mixed-effects regression model.
Results
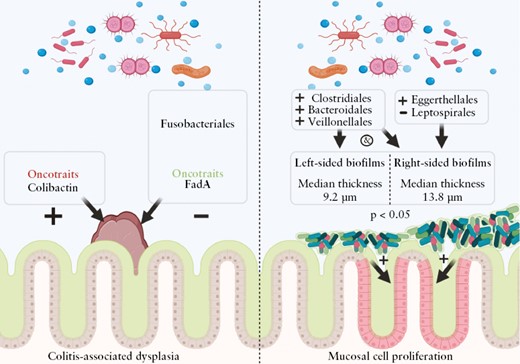
Biofilms were highly prevalent in UC patients [90.8%] with a median persistence of 3 years (interquartile range [IQR] 2–5 years). Biofilm-positive biopsies showed increased epithelial hypertrophy [p = 0.025] and a reduced Shannon diversity independent of disease status [p = 0.015], but were not significantly associated with dysplasia in UC: adjusted odds ratio [aOR] 1.45, 95% confidence interval [CI] 0.63–3.40. In contrast, ClbB independently associated with dysplasia [aOR 7.16, 95% CI 1.75–29.28], and FadA and Fusobacteriales were associated with a decreased dysplasia risk in UC [aOR 0.23, 95% CI 0.06–0.83, p <0.01].
Conclusions
Biofilms are a hallmark of UC; however, because of their high prevalence are a poor biomarker for dysplasia. In contrast, colibactin presence and FadA absence independently associate with dysplasia in UC and might therefore be valuable biomarkers for future risk stratification and intervention strategies.